What is ketoacidosis? It is a lethal condition responsible for over 100,000 hospital admissions per year in the US, with a death rate of around 5%.
Why does this happen? Because of a deadly combination of uncontrolled hyperglycemia, increased blood ketone levels, and metabolic acidosis.
Luckily, this lethal triad rarely affects individuals who don’t have diabetes. That said, the majority (80%) of ketoacidosis cases occur in people with a known history of diabetes mellitus (any form of diabetes).
To help you develop a better understanding of ketoacidosis and how it relates to your health, let’s examine the following topics:
- Ketoacidosis defined
- The difference between ketoacidosis and diabetic ketoacidosis
- The three types of ketoacidosis
- What is the most common cause of ketoacidosis?
- Ketoacidosis symptoms
- How to test for it
- Short-term DKA prevention tips
- Long-term prevention strategies
- Keto and diabetes
- Is it a keto concern? nutritional ketosis vs. ketoacidosis
- More natural ways to control your blood glucose levels
- Key takeaways
What is Ketoacidosis?
Ketoacidosis is when the body produces abnormally high levels of ketones while blood sugar is also too high, resulting in a drop in blood pH and metabolic acidosis. Since the body relies on a specific pH range to function, metabolic acidosis is potentially lethal if left untreated.
Fortunately, this only occurs under abnormal metabolic conditions. The most common cause being uncontrolled type 1 diabetes, which creates the ideal metabolic environment for diabetic ketoacidosis.
Ketoacidosis vs. Diabetic Ketoacidosis — What’s The Difference?
At this point, you may have noticed that ketoacidosis and diabetic ketoacidosis are often used interchangeably. This is because it is difficult for the body to get into a state of ketoacidosis without the blood glucose control issues that are common in people with diabetes. Hence, the term diabetic ketoacidosis.
(That said, there are other less common forms of ketoacidosis as well, which we will learn about in the next section.)
Ketoacidosis tends to occur the most in people who have type 1 diabetes. Somewhere between 5 and 8 of every 1,000 people with type 1 diabetes develop diabetic ketoacidosis each year.
People with type 2 diabetes also run the risk of ketoacidosis under stressful situations. Still, it is much less common since they have some remaining insulin production (type 1 diabetics do not).
If you are not part of the 422 million people worldwide that have diabetes, your risk of getting ketoacidosis is negligible. You would have to put yourself through excessive stress, unhealthy eating habits, and/or chronic alcohol abuse before experiencing ketoacidosis.
The Three Types of Ketoacidosis
Ketoacidosis only occurs under abnormal metabolic conditions — The most common being uncontrolled diabetes. The other two types can result from chronic alcoholism or starvation under stressful conditions.
Here’s a quick overview of the three:
- Diabetic ketoacidosis (DKA) — When diabetes isn’t being controlled by insulin injection, medication, and/or proper lifestyle changes, blood sugar, and blood ketone levels can rise exponentially. If left untreated, this metabolic state of acidosis can lead to diabetic coma and death.
- Alcoholic ketoacidosis (AKA) — Chronic alcoholism can disrupt your body’s function so much that it enters a state of excessive ketone body production, dehydration, and blood sugar level dysregulation, which can bring the body into ketoacidosis.
- Starvation ketoacidosis (SKA) — Long bouts of starvation combined with excessive stress are known to cause ketoacidosis, particularly for conditions such as pregnancy, eating disorders, and extreme exercise. Simply put, SKA can occur when a sustained severe calorie deficit meets excessive physical and/or emotional stress.
Although each type has a different trigger, they all result from a combination of uncontrolled blood sugar levels, a sharp rise in ketone bodies, and metabolic acidosis. To give us a better idea of why this happens, let’s take a closer look at the mechanism behind DKA.
How Does Diabetic Ketoacidosis Happen? The Underlying Cause
The common consensus in the scientific community is that the primary underlying cause of ketoacidosis is insulin deficiency. This can be caused by being born without the ability to produce enough insulin (type 1 diabetes) or living a lifestyle that promotes insulin resistance (type 2 diabetes).
When a person has insulin deficiency, their liver and fat cells aren’t listening to and/or receiving the signal from insulin that the body has excess energy. This will trigger the fat cells and liver cells to go into starvation mode, even after a calorically dense meal.
The fat cells begin to dump triglycerides into the blood to provide the other cells with energy (one of the reasons why some people have high triglyceride levels on their blood test).
Meanwhile, the liver will start mobilizing stored glycogen and using gluconeogenesis and ketogenesis to provide the body with sugar and ketones that it doesn’t really need.
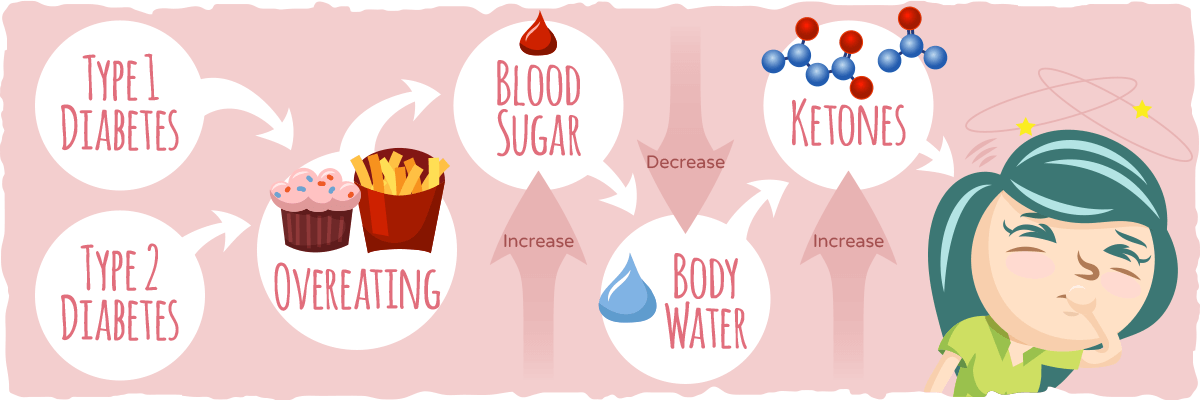
All of this causes blood sugar to rise to unhealthy levels (uncontrolled hyperglycemia), while the lack of insulin efficiency allows ketones to build up in the blood. The excess sugar and ketones will then start to draw water out of the tissues, into the blood, and out of the body in the urine.
With less water in the blood (due to frequent urination), the acidity of the ketones makes the blood so acidic that the body enters a state called “metabolic acidosis.”
In other words, the blood becomes so acidic that the body cannot function properly. This causes many of the common ketoacidosis symptoms that people with diabetes should look out for.
The Symptoms of Ketoacidosis
Ketoacidosis usually develops rapidly (within a time span of 24 hours). The most prevalent symptoms are vomiting and abdominal pain (which are especially common in children with ketoacidosis). People who are experiencing ketoacidosis will also be dehydrated and have low blood pressure, higher blood glucose, and a higher heart rate.
It is also important to be aware of the person’s mental state. In mild ketoacidosis, patients will tend to be alert. As ketoacidosis worsens, the patient will start to feel drowsy and may even lose consciousness. At its most severe, ketoacidosis can put the patient in a coma.
Here is a quick overview of the most common ketoacidosis symptoms:
- Vomiting
- Abdominal pain
- Dehydration
- Drowsiness
- Blood glucose that is above 250 mg/dl
- Blood pressure that is less than 90/60
- Resting heart rate above 100 beats per minute
If you have most of these symptoms and you have diabetes, then it is highly likely that you are in ketoacidosis. However, you will not know for certain if you have some of the symptoms of ketoacidosis unless you test for them first.
How to Test For Ketoacidosis Symptoms
Vomiting, abdominal pain, and drowsiness are self-explanatory, but they can be attributed to many other issues as well. This is why it is important to check for the other symptoms of ketoacidosis before you rush to the hospital.
To See if You Are Dehydrated:
Dehydration can be tested by pinching the skin on the part of your forehead just above and between your eyebrows called the glabella.
Does the skin recoil right back after you release it or stay folded for a couple of seconds? If it stays folded, then you are dehydrated.
Here is a more specific breakdown of what your findings mean:
- The skin that, after being pinched and released, goes back to its original position immediately suggests good hydration.
- A skin fold persisting for less than 2 seconds suggests mild dehydration.
- A skin fold persisting for 2-10 seconds speaks for moderate dehydration.
- A skin fold persisting for several seconds or even minutes speaks for severe dehydration.
To Test Your Heart Rate:
First, make sure you are relaxed and fully recovered from activity before you measure your heart rate.
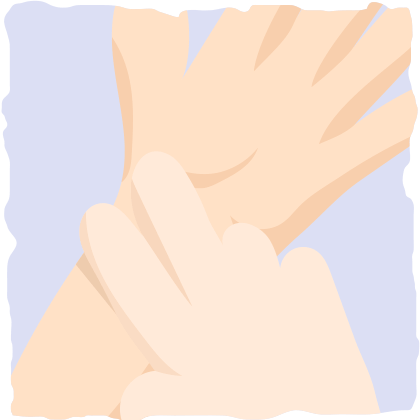
Check your pulse at your wrist by placing two fingers between the bone and the tendon over your radial artery (it is located on the thumb side of your wrist).
Start a stopwatch and count how many pulses (heartbeats) you feel under your fingers for 15 seconds and multiply it by 4. This is your heart rate.
For example, if you count more than 25 beats in 15 seconds then your heart rate is above 100 per minute.
To Check Your Blood Pressure:
Most of us don’t have a blood pressure cuff lying around at home, so if you have a combination of these symptoms then your blood pressure might be low:
- Dizziness or lightheadedness
- Fainting
- Blurred vision
- Nausea
- Fatigue
- Lack of concentration
To Check Your Blood Sugar Levels:
Blood glucose meters are cheap and easy to get nowadays. If you have diabetes or if you are concerned about your blood sugar levels, then it is a good idea to get one.
All it takes is a finger prick and a drop of blood, and you’ll have your blood sugar reading. If your blood sugar is above 250 mg/dl, and you have most of the other symptoms on the list, then it is highly likely that you have ketoacidosis.
For those who do not have a glucose meter, here are common symptoms of hyperglycemia (high blood sugar):
- Increased thirst
- Headaches
- Trouble concentrating
- Blurred vision
- Frequent peeing
- Fatigue (weak, tired feeling)
Checking for all of the symptoms of ketoacidosis will take less than 5 minutes, and it will let you know if you may be experiencing the effects of this lethal triad. But what do you do if you have almost all of the ketoacidosis symptoms? Drink plenty of water with a pinch of salt in it, follow the treatment program suggested by your doctor, and continue reading this article.
Short-term Prevention of Ketoacidosis
A study on diabetic ketoacidosis published in 2012 indicates that approximately 50% of hospital admissions due to ketoacidosis are preventable with improved outpatient treatment programs and better adherence to self-care.
This can mean many things, but the authors of the study suggest that diabetics should monitor their blood sugar levels throughout the day and administer their insulin and medication when necessary. That’s it — preventing ketoacidosis is that simple.
However, these guidelines don’t address the millions of people that have blood sugar control issues but have no insulin or medication to help them. What should they do?
If you are experiencing mild ketoacidosis symptoms currently, then you must go to the doctor and be put on an appropriate blood sugar control program. Drink water with a pinch of unrefined salt in it and don’t eat anything on the way to the doctor so the symptoms don’t get worse.
On the other hand, if you don’t have any symptoms of ketoacidosis, but you want to prevent it from happening, there is an even better approach.
Long-Term Prevention of Ketoacidosis and Its Symptoms
The key to preventing ketoacidosis is insulin efficiency. This means that you have adequate insulin, and your cells respond to it when it is released. When insulin is functioning properly, ketones and blood sugar can never build up in the blood and cause ketoacidosis.
The best way to improve insulin efficiency is with exercise and the right diet. The concept of exercising to prevent ketoacidosis is easy enough. Simply by moving more, you will cause the cells in your body to be more responsive to insulin and your blood sugar levels to be more stable. If you move more with more intensity (e.g., lifting heavy weights, CrossFit, sprinting), you will improve insulin efficiency even more.
Dieting to avoid ketoacidosis, however, is a bit more complicated (at first). Following the typical western diet can easily result in blood sugar control issues, so we need better guidance. Fortunately, many research studies have found that a handful of diets can help improve blood sugar levels and reduce insulin resistance. For example, calorie restriction, the low glycemic index diet, and the ketogenic diet have all been found to improve blood sugar levels.
However, one of these diets has been proven to be much more effective than the other two. In fact, it is so effective that it can help reverse diabetes.
The Ketogenic Diet and Diabetes
In a recent study that put the ketogenic diet up against a calorie-restricted low-glycemic index diet, the ketogenic diet was more effective at improving diabetes-related markers. Many subjects who were on the ketogenic diet were also able to reduce their diabetes medications during the study. Because of these tremendous results, the researchers concluded that “lifestyle modification using low carbohydrate interventions is effective for improving and reversing type 2 diabetes.”
These findings were confirmed by another study that put 21 diabetic subjects on the ketogenic diet. In this study, most of the 21 subjects reduced or discontinued their diabetes medications. The researchers concluded that “the LCKD [Low-Carbohydrate Ketogenic Diet] can be very effective at lowering blood glucose.”
However, it is important to remember that these are only two studies that were conducted on small groups of people. In order to draw accurate conclusions, we need to examine more studies. (Luckily for us) This is exactly what a group of 26 leading researchers did. They dug through most of the data on carbohydrate restriction in managing diabetes and concluded that there is:
…evidence supporting the use of low-carbohydrate diets as the first approach to treating type 2 diabetes and as the most effective adjunct to pharmacology in type 1. They represent the best-documented, least controversial results.
In other words, if you have type 1 or type 2 diabetes then you should be on a low-carbohydrate diet. But what does this have to do with ketoacidosis?
A Keto Concern? Nutritional Ketosis vs. Ketoacidosis
One of the main purposes of the keto diet is to get into nutritional ketosis (i.e., using ketone bodies as a primary energy source). This may sound like a terrible idea after learning that increasing blood ketone levels can lead to metabolic acidosis, but keep in mind that this only occurs under abnormal metabolic conditions.
In fact, following a keto diet can actually help prevent DKA by keeping blood sugar levels under control. This is because sustained ketosis can only be achieved when restricting carbohydrates. Without carbohydrates, the cells become more sensitive to insulin, making insulin more efficient.
After around three days of carbohydrate restriction, the cells are forced to shift into a fat- and ketone-burning mode. The liver creates ketones and the fat cells release triglycerides to be used as fuel.
This is a similar process to what happens before the body goes into ketoacidosis, but with one important difference: During carbohydrate restriction, blood glucose and insulin levels are under control.
With blood sugar at healthy levels and insulin working efficiently, ketone levels will not get too high because the liver now has an accurate idea of how much is needed to fuel the body. This allows the liver to decrease ketone production before metabolic acidosis occurs (which is when ketone levels are around ten times the levels you can achieve with keto).
To make a long story short: By preventing, managing, or reversing diabetes with a low-carb keto lifestyle, you can avoid diabetic ketoacidosis as well.
Other Natural Ways to Prevent Ketoacidosis and Diabetes
Exercise is one of the simplest ways to lower your blood sugar levels now and in the future. One study found that going for one 25-60 minute run can improve insulin sensitivity for up to 5 days (in younger women). Resistance training seems to have similar (if not better) effects as well.
In general, if you move more, your body will need to use more energy. The more energy your body uses, the more it will need to increase insulin sensitivity in the cells that need it most (i.e. your muscle cells). This is essential for promoting health and preventing diabetes and ketoacidosis.
Start with whatever activities you enjoy doing and make it a bit more challenging.
If you like going for walks, then see if you can walk a bit faster or up more hills. If you like to lift weights, then increase the volume or the intensity. If you don’t like doing any form of activity, then go for a short walk. Any activity is good (as long as you don’t do too much at once).
Another way to prevent ketoacidosis is to reduce stress. Whether you are stressed because you are being attacked by a snake or because you have a fear of snakes that was triggered by reading the word “snake”, stress hormones are released into your bloodstream. These stress hormones trigger a rise in blood sugar levels and an increase in insulin resistance. If the short-term stressor doesn’t go away and you are stressed most of the time, then your likelihood of getting type 2 diabetes and ketoacidosis raises dramatically.
There are many tools you can use to relieve stress, but meditation (not medication) and deep breathing are the healthiest and most reliable. Meditation, by itself, can help reduce blood sugar and stress levels. When you combine meditation with slow, deep breaths into your abdomen, your stress response will melt away.
Key Takeaways: Ketoacidosis, Ketosis, and Your Keto Lifestyle
Ketoacidosis is a serious issue that can become lethal, but it is preventable (in most cases). It occurs when blood sugar levels and ketone levels are simultaneously too high. As a result, common ketoacidosis symptoms like vomiting, abdominal pain, dehydration, hyperglycemia, hypotension, tachycardia, and drowsiness can occur.
Ketoacidosis almost exclusively affects those with diabetes who aren’t mindful of their blood sugar levels and medication. This is why the best short-term prevention strategy is to monitor blood glucose levels and take diabetes medication when necessary.
If you have diabetes and you’re experiencing almost all of the symptoms of ketoacidosis right now, then it is best to go to the doctor (or the hospital if you are continuing to get worse).
For those of you concerned about getting ketoacidosis in the future, there is no need to worry! You can prevent ketoacidosis completely by making simple lifestyle adjustments.
The most effective prevention strategies are exercising regularly, meditating with deep breathing, and restricting dietary carbohydrates with a low carb or keto diet.
To help you make a seamless transition into a lower carb lifestyle, check out the resources below:
- Comprehensive Keto Beginner’s Guide — Everything you need to know about keto eating in one place.
- Keto Calculator — Learn exactly how much you should eat to promote ketosis and reach your goals.
- The Keto Meal Plan App — No-fuss personalized meal planning, just cook and eat.
Sources:
- Diabetic Ketoacidosis — Deep Dyve
- The Metabolic Derangements and Treatment of Diabetic Ketoacidosis — NEJM
- Diagnosis and treatment of diabetic ketoacidosis and the hyperglycemic hyperosmolar state — CMAJ
- Diabetic Ketoacidosis: A Review and Update — Springer Link
- Diabetes — World Health Organization
- Hyperglycemic Crises in Adult Patients With Diabetes — American Diabetes Association
- What Can I Eat? — Diabetes
- Relaxation techniques: Breath control helps quell errant stress response — Harvard Health Publications
- Effects of mindfulness meditation on serum cortisol of medical students. — NCBI
- Hyperglycemic Emergencies — Diabetes in Control
- Diabetic Ketoacidosis and Hyperglycemic Hyperosmolar Syndrome — American Diabetes Association
- The Physiology of Stress: Cortisol and the Hypothalamic-Pituitary-Adrenal Axis —Dartmouth Undergraduate Journal of Science
- Cortisol Is Negatively Associated with Insulin Sensitivity in Overweight Latino Youth — NCBI
- How do I increase insulin sensitivity? — Examine
- Aerobic training improves insulin sensitivity 72-120 h after the last exercise session in younger but not in older women. — NCBI
- Improvement of obesity-linked skeletal muscle insulin resistance by strength and endurance training. — NCBI
- Dietary carbohydrate restriction as the first approach in diabetes management: Critical review and evidence base — Nutrition Journal
- Low carbohydrate diet in type 1 diabetes, long-term improvement and adherence: A clinical audit — NCBI
- The effect of a low-carbohydrate, ketogenic diet versus a low-glycemic index diet on glycemic control in type 2 diabetes mellitus. — NCBI
- A low-carbohydrate, ketogenic diet to treat type 2 diabetes — NCBI
- Diabetic ketoacidosis — Medline Plus
- Resistance Training and Type 2 Diabetes — American Diabetes Association
- Starvation ketoacidosis – a rare but significant metabolic condition — Society for Endocrinology
- Ketoacidosis — NCBI Bookshelf








Hi,
I’m a 48 y.o. male ultra endurance cyclist who has just been diagnosed with Type 1` Diabetes.
I’m looking at Keto diet as an adjunct to the insulin treatment I will need to help keep my blood glucose under control.
Above in the section on Ketoacidosis and Diabetes, you mention some a study by 26 researchers on low carb & diabetes – is it possible to send me a link to the source material or some other way for me to be able to access this material?
Thanks,
David
Hey David,
I believe this is the study you are looking for:
http://www.abc.net.au/catal…
If you want more specific info regarding type 1 diabetes and keto, I recommend reading through this article instead:
https://www.ruled.me/type-1…
If you have any other questions, please let me know.